This is the fourth profile in a GW Today series featuring faculty from the Columbian College of Arts and Sciences and the School of Engineering and Applied Science who are conducting research with an impact in Science and Engineering Hall.
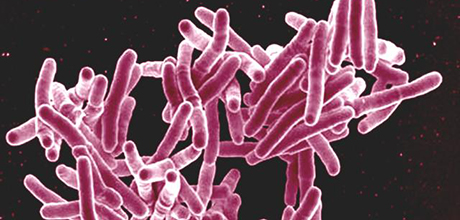
Tuberculosis (TB)? Didn’t we cure that a while ago? The short answer, says George Washington University Chemistry Professor Cynthia Dowd, is a definitive “no.”
In 2013, the disease—signs of which have been found in Egyptian mummies from 2400 B.C.— infected 9 million people worldwide and killed 1.5 million, according to the World Health Organization (WHO). It is second only to HIV/AIDS as the greatest killer worldwide due to a single infectious agent.
A six-month course of antimicrobial drugs can kill TB, which spreads from bacteria released in the air when an infected person coughs or sneezes. But the disease is evolving faster than available antibiotics can keep up.
“Drug resistance is absolutely on the rise globally and in the U.S.,” said Dr. Dowd, a medicinal chemist who joined the Columbian College of Arts and Sciences in 2007. “And it’s just going to get worse.”
Though the number of TB cases reported annually in the United States has decreased since a resurgence peak in 1992, a lack of access to treatment and diagnosis in poorer countries is blocking efforts to eradicate the disease. New resistant strains of TB are emerging in many parts of the world.
“Now with global travel, people are taking the disease with them,” Dr. Dowd said.
Though TB and other types of once-treatable bacteria quickly are evolving, drug development is lagging behind. Only in the past decade have there been significant strides in TB drug development and discovery since the 1970s. Spurred on by rises in resistance and HIV-TB co-infection, this period of TB research is resulting in new antibiotics that are slowly making their way through the drug discovery pipeline and becoming available for patients.
As TB continues to fight back, Dr. Dowd is on a mission to develop new small molecule inhibitors that will stop the disease in its tracks.
A Complicated History
The story of TB in the United States is one that rises and falls.
Once the leading cause of death in the United States, TB cases had dropped dramatically by the second half of the 20th century. Then, in the mid-1980s, HIV hit. And TB made an unexpected comeback.
An HIV-TB co-infection is “a really scary combination,” said Carl Brothers, a fifth-year Ph.D. student in the Dowd lab. HIV patients have weakened immune systems, making them up to 30 times more likely to contract TB or to activate latent TB, which hides symptomless in the body. At least one-third of people living with HIV worldwide in 2013 were infected with TB, and it is one of the leading causes of HIV-related death. On top of that, HIV and TB drugs are often incompatible, so the drugs for one disease may kill or change the effects of the drugs needed for the other.
The reemergence of TB in HIV patients worldwide was the catalyst for drug-resistant forms of TB to emerge.
In 2005, at the Church of Scotland Hospital in Tugela Ferry, a rural and poor area in South Africa, HIV patients who had been responding well to drugs began dying rapidly from TB. South African and U.S. researchers discovered that 221 of the 542 TB patients had a multi-drug-resistant form (MDR) of the infection, which would not respond to typical drug therapies.
Worse, 53 of those patients did not respond to a second line of antibiotics that could treat MDR. It marked the first major outbreak of what became known as extensively drug-resistant (XDR) TB.
“TB is kind of like super bacteria. A number of antibiotics are ineffective against it,” Mr. Brothers said. “Then on top of that, it’s developing resistance to the few that you have to treat it.”

Ph.D. student Carl Brothers uses synthetic organic chemistry to make and evaluate molecules against biochemical targets in Dr. Dowd's Science and Engineering Hall lab. (William Atkins/GW Today)
Multidrug-resistant TB is not only challenging, but also extremely expensive to treat. In 2010, direct costs ranged from $17,000 to treat drug-susceptible TB to $430,000 to treat the most drug-resistant form of the disease (XDR-TB), according to the Centers for Disease Control and Prevention.
In 2013, WHO estimates that 480,000 people worldwide developed MDR-TB, and about 9 percent of these cases were XDR-TB. Multidrug-resistant TB remains rare in the United States, where there were 63 cases of XDR-TB reported between 1993 and 2011.
“While TB is not a huge threat in the U.S. yet, we have had cases of multi-drug resistant and extensively drug resistant TB,” Mr. Brothers said.
And, he noted, the bacteria is not resting. “We need new drugs for TB—now,” he said.
A Hidden Killer
Compounding this issue, Dr. Dowd explained, roughly one-third of the world’s population has latent TB infections. Latent TB can live hidden and symptomless in the body. Those with this type of bacteria do not know they are sick and cannot spread the infection to others. However, if the TB bacteria become active, caused by a weakened immune system, the infected person will become sick.
Since most first-line antibiotics are effective only against actively growing bacteria and not latent bacteria, this is hindering opportunities to decrease TB cases worldwide. To treat the disease fully, researchers will need to identify agents that will kill both active and latent bacteria, according to Dr. Dowd.
Active bacteria produce enzymes that catalyze life-sustaining tasks, such as DNA replication.
While enzyme inhibitors stop these metabolic processes from beginning and kill active TB bacteria, they are ineffective against latent bacteria, which have reduced metabolism.
The major challenge in developing new TB drugs, Dr. Dowd said, is to identify specific metabolic processes that are required for cells to maintain life in latent bacteria. Her group’s long-term goal is to understand which processes are essential for Mycobacterium tuberculosis to survive in a dormant state. The researchers do this by developing and testing small chemical tools, or enzyme inhibitors, and examine their effect on the bacteria’s survival.
In the “lock and key” analogy commonly used to describe drug design, Dr. Dowd’s job is to design molecules or “keys,” which target specific enzymes or “locks” that drive life-sustaining biochemical reactions.
“Every cell has a specific chain of events that have to happen in order for the cell to grow and survive,” Dr. Dowd said. “We’ve zeroed in on one step in the process for TB to survive. And once you kill that step, the whole pathway shuts down.”
Dr. Dowd and her research team investigate potential new targets in the fight against TB.
A little more than a decade ago, researchers discovered a new metabolic pathway in cells, called the nonmevalonate pathway, which does not exist in humans, but has been shown to be essential for survival in M. tuberculosis. It makes it an attractive target for therapeutic intervention.
“This is really exciting, because we can make drugs that will kill bacteria but are less likely to hurt humans,” Mr. Brothers said.
Dr. Dowd and her team’s current work focuses on stopping an enzyme abbreviated as Dxr, which is part of this nonmevalonate pathway.
Described in a 2012 paper, the GW researchers designed and tested molecules (or keys) that blocked two binding sites, or “locks,” on the Dxr enzyme: NADPH and fosmidomycin. To do this, they first had to mask the molecules, enabling the inhibitors to sneak past the bacteria’s defenses, like a chemical Trojan horse.
The successful work marked the first time that the Dxr has been used to kill TB and could potentially kill dormant TB infections, since the enzyme is involved in the basic-level cell functions.
Now Dr. Dowd and her team are combining the "Trojan horse" idea with a variety of hypotheses about Dxr inhibition. By making small changes in the inhibitors, her group is learning which structural elements are beneficial for shutting down the enzyme.
“We have to keep refining the key, making it the best it can be to fit the lock,” Dr. Dowd said. “It’s a long process, but we’re getting better at it.”