The year 2020 marked a decade of developments in cardiac optogenetics, a biological technique combined with optics, whereby light is used to control cells in living tissue, in this case the heart, that have been genetically modified to express light-sensitive ion channels.
George Washington University School of Engineering and Applied Science researchers Emilia Entcheva and Matthew Kay, both professors in the Department of Biomedical Engineering, are leaders in the field of cardiac optogenetics. They recently published a review in Nature Reviews Cardiology that examines advancements made over the past 10 years—and discusses challenges and opportunities that lie ahead.
Dr. Entcheva and Dr. Kay spoke with GW Today about their review and the impact of developments in the field:
Q: What do you think is the most transformative development in the field of cardiac optogenetics in the past 10 years?
Dr. Kay: The field of cardiac optogenetics is itself a transformative development. Before the demonstration that cardiac tissue could be stimulated using light, electrical current was thought to be the primary mode for pacing and defibrillating the heart. Cardiac optogenetics now provides an entirely new way to control heart rhythm, and it is being used increasingly more often in basic science investigations of arrhythmias and in high-throughput screening platforms using cultured cardiac cells and tissue.

Clockwise: Julie Han, Christianne Chua, Gantt Meredith, Maria Pozo, Dr. Wei Liu, Dr. Emilia Entcheva; virtually on screen: Michael Pressler and Weizhen Li.
Q: How have the developments in this field changed the conversation about cardiac issues such as arrhythmias?
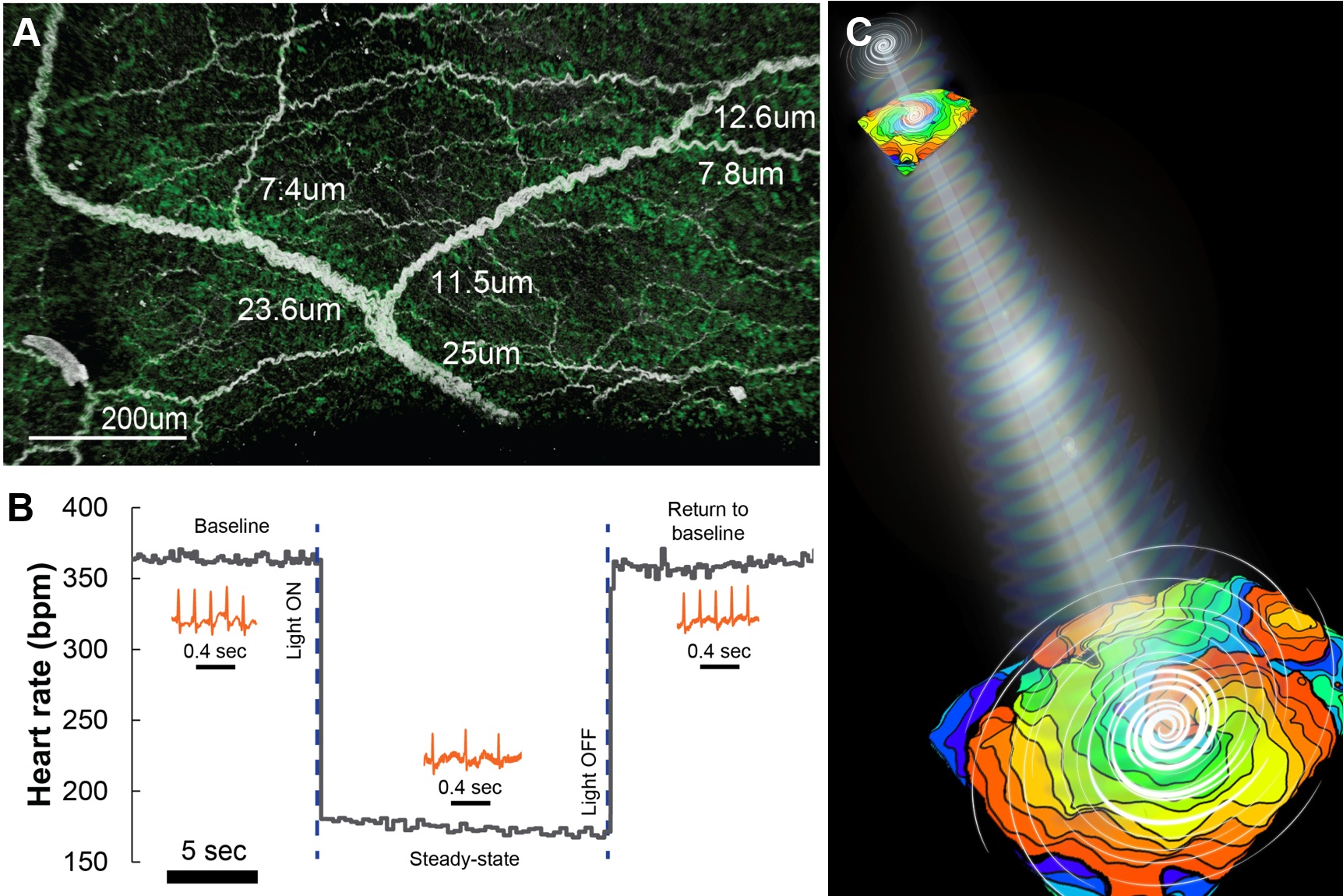
Dr. Entcheva: Several years ago, in collaboration with other researchers, we demonstrated a conceptually new way for arrhythmia control called “wave steering,” where a dynamic optical stimulation pattern can re-shape the path of an excitation wave—sort of like steering a ship from troubled waters into safer space. This is not currently part of the design of cardiac devices such as pacemakers and defibrillators. This concept could revise our view on arrhythmia ablation as well—with gentler, tissue-sparing methods to terminate life-threatening events with a perturbation that requires very little energy and is pain-free for the patient.
Q: What role have GW researchers played in pushing the field forward?
Dr. Entcheva: About 10 years ago, my laboratory was among the first to demonstrate utility of optogenetic tools in cardiac tissue. We developed mathematical models of how these light-driven perturbations compare with classic electrical stimulation and highlighted what added benefits they may provide. Our focus, experimentally, was to integrate high-resolution optical mapping with spatiotemporal optical stimulation, thus to develop a fully all-optical framework to study cardiac electrophysiology. We envisioned the immediate impact to be in high-throughput platforms for drug screening and cardiotoxicity testing using human stem-cell-derived cardiomyocytes, and we have contributed to the development of such systems.
Dr. Kay’s lab work in cardiac optogenetics has provided the first publications describing the effect of cell-type specific optogenetic activation of the autonomic neurons within the heart. His first publication in the field presented how the cardiac flight-or-fight response could be instantly activated by shining light on the surface of the heart. Recent work has provided new insights in the field of neuro-cardiology by robust optical modulation of heart rate by light.

Members of Dr. Kay's lab: Jeannette Rodriguez Gonzalez (top left), Rebekah Russo, Grey Harral, Makeda Melkie, Grant Kowalik, Emily Cheung, Bridget Alber, Aman Gill.
Q: What are the barriers that can make it a challenge to translate laboratory developments to clinical applications?
Dr. Kay: One important barrier is to provide “disruptive technology” to the current state-of-the-art in clinical cardiac devices. For a new technology to be widely adopted it must be more effective and safer than current solutions. This can be a high barrier to overcome in the field of cardiac devices, which have evolved and have been perfected over numerous decades. Yet, extended battery life, painless lower-energy defibrillation and other features to improve a patient’s quality of life may be better addressed using cardiac optogenetics, as gene therapy approaches improve. More immediately, the technology is already poised to have a major impact in the field of personalized medicine, high throughput screening of cardiac drugs and informing the intelligent design of new implantable cardiac devices.
Q: How do you think cardiac optogenetics will change in the next 10 years?
Dr. Entcheva: As discussed in our review, within the next 10 years we envision near-time impact in high-throughput screening platforms for drug development and personalized medicine.
Long-term developments that could enter the clinic and may need 10 more years of work, have to do with smarter ways to control arrhythmias. Atrial arrhythmias are more forgiving—a failure of intervention is not fatal. They are more likely to benefit early on from optogenetic or optogenetics-inspired termination approaches that, in contrast to current ablation, would be tissue-sparing. The possibility for genetic targeting of specific cell types likely will be leveraged for precise neuro-cardiac intervention—i.e. optogenetic autonomic control, derived from pioneering work done at GW in Dr. Kay’s lab. Optogenetics-inspired control strategies, such as “wave steering” likely will make their way into implantable devices with multi-site access to the heart surface.
If photonics-based devices are to replace current-day pacemakers and defibrillators, they may be powered by biologically-generated light, such as bioluminescence. Many electrical circuit-based concepts are implementable in biological media using synthetic biology. Cardiac optogenetics will likely evolve in a synergistic partnership with smart biophotonics-relevant materials and protein engineering to provide new functionality to cardiac muscle for therapeutic purposes.