A research team led by scientists at George Washington University has developed two mRNA vaccines that are highly effective in the fight against malaria, reducing both infection and transmission.
Malaria is a scourge affecting more than 90 countries around the world, causing 241 million cases and an estimated 627,000 deaths every year. An effective vaccine for the disease has long been elusive, but recent advances in the development of vaccines such as the mRNA vaccines for SARS-CoV2 could lead to a new generation of powerful anti-malaria weapons.
“Malaria elimination will not happen overnight but such vaccines could potentially banish malaria from many parts of the world,” said Nirbhay Kumar, a professor of global health at GW’s Milken Institute School of Public Health. “The mRNA vaccine technology can really be a game changer. We saw how successful this technology was in terms of fighting COVID and for this study we adapted it and used it to develop tools to combat malaria.”
The team found that two experimental vaccines induced a powerful immune response regardless of whether they were given individually or in combination. The study, supported by the National Institutes of Health, was published in the Dec. 1 issue of npj Vaccines, an open-access scientific journal.
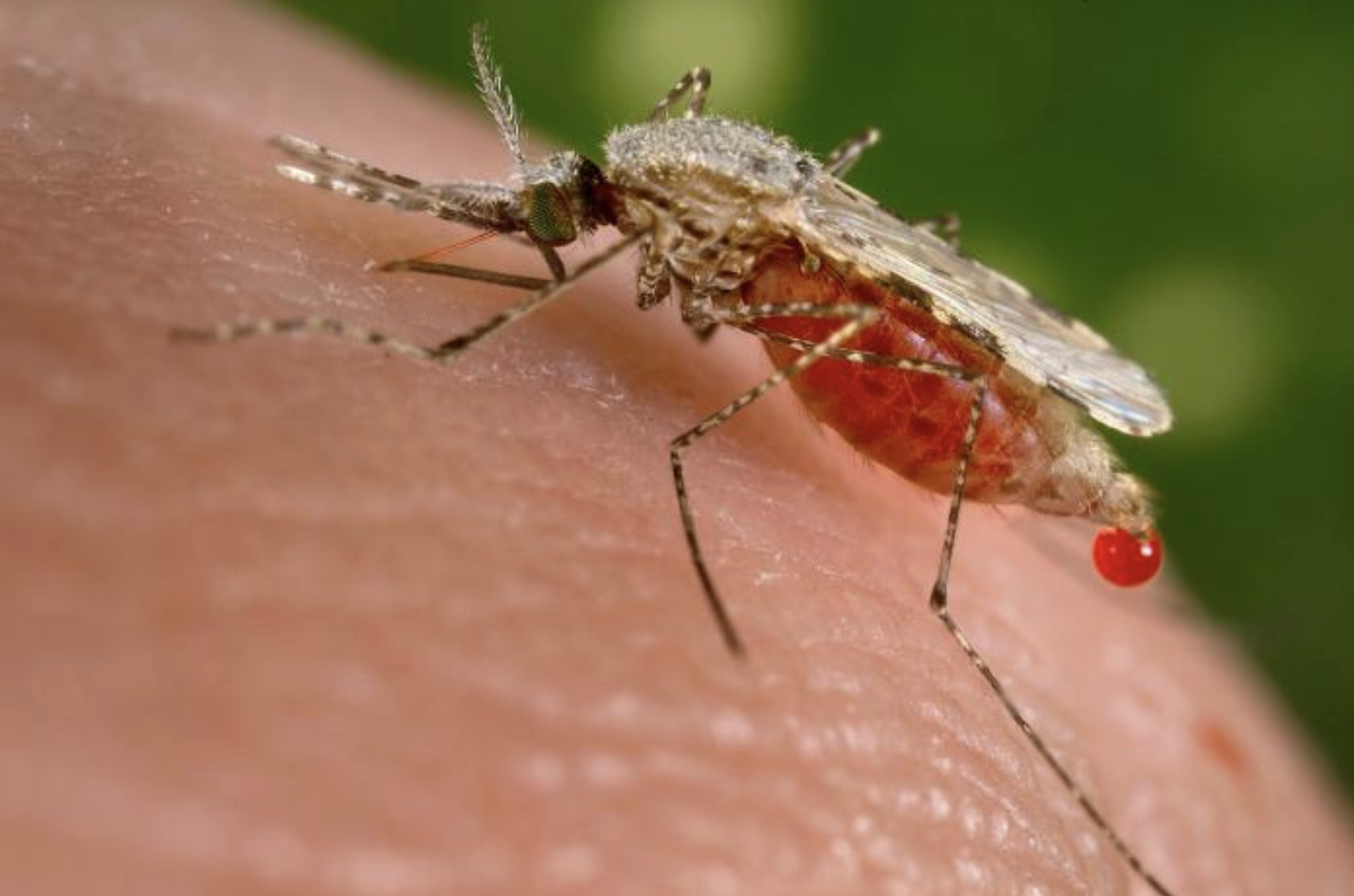
Kumar and the research team focused on the parasite Plasmodium falciparum, one of four parasite species that cause malaria. Transmitted through the bite of the Anopheles mosquito, P. falciparum together with P. vivax are responsible for more than 90% of all malaria cases globally, and 95% of all malaria deaths. Most cases and deaths occur in sub-Saharan Africa but half the world’s population is at risk of contracting this deadly disease. Kumar’s team developed two mRNA vaccines to disrupt different parts of the parasite’s life cycle.
The researchers immunized one group of mice with a vaccine targeting a protein that helps the parasites move through the body and invade the liver. They immunized another group of mice with a vaccine targeting a protein that helps parasites reproduce in a mosquito’s midgut.
Both vaccines induced a potent immune response. The presence of protective antibodies during transmission of parasites to healthy mosquitoes dramatically reduced the parasite load in the mosquitoes, an important step in disrupting malaria transmission, according to the researchers.
“These vaccines were highly effective at preventing infection and they wiped out transmission potential almost entirely,” Kumar said.
The team also immunized mice with both vaccines together and found that co-immunization effectively reduced infection and transmission without compromising the immune response.
The vaccines were developed in partnership with scientists from the University of Pennsylvania and other collaborators. The team has filed for a patent, and its members hope to usher their vaccines through additional research, including studies in nonhuman primate models, with the goal of producing vaccines that can be used safely in humans.
“To have a vaccine cocktail that can effectively disrupt multiple parts of the malaria parasite’s life cycle is one of the holy grails of malaria vaccine development,” Kumar said. “This study brings us one step closer to producing vaccines that can be used safely in humans to prevent illness and save lives, with the ultimate goal of defeating this disease.”