Her bosses at the Centers for Disease Control and Prevention told Lauren Epstein, B.S. ’03, M.D. ’07, she had two hours to pack her bags before boarding a plane to Dallas on the afternoon of Sept. 30.
The George Washington University double alumna arrived in Dallas at 11 that night. The next morning, Dr. Epstein headed to Texas Health Presbyterian Hospital where Thomas Eric Duncan, the first patient diagnosed with Ebola in the United States, died two weeks ago.
 |
| Lauren Epstein |
Dr. Epstein is a member of the CDC’s Epidemic Intelligence Service, a two-year post-graduate training program for health professionals interested in applied epidemiology. As part of a health care contact tracing team, she is one of about a dozen “disease detectives” sent to Texas Health Presbyterian to identify and monitor health care workers who came into contact with Mr. Duncan while he was infected with Ebola.
An expert in infectious diseases, Dr. Epstein is no stranger to responding to crises. She has led outbreak investigations of drug-resistant organisms in hospitals, including an E. coli outbreak associated with specialized gastrointestinal endoscopes in Illinois.
But in Dallas, the stakes—and the pressures—were higher. Hospital workers were “very scared,” she said. Helicopters circled the hospital, news vans lined the sidewalks and video cameras followed Dr. Epstein into work each morning.
“The whole world was watching,” said Dr. Epstein, who returned to CDC headquarters in Atlanta on Tuesday after three weeks in Texas. “Seeing the challenges you’re dealing with every day on the front pages of newspapers is…surreal.”
Still, she tried to ignore the buzz. She had a job to do.
“You kind of have to keep your head down and not focus on all the things happening around you,” Dr. Epstein said. “I am very comfortable working in hospitals, and I felt confident that I knew what to do. But having all eyes looking at me was something I had never experienced before.”
While in Dallas, Dr. Epstein worked with hospital leadership to compile a list of any health care workers who could have had contact with Mr. Duncan. Her team then interviewed each person and identified which workers could have been exposed to the Ebola virus. When she found someone who could pose a high risk, she monitored him or her for fever and other Ebola symptoms over the following days.
“We had to cast a wide net. We were not just thinking about doctors and nurses, but also lab techs, radiologists—really anyone who could have been exposed to the sick patient,” she said.
Other members of the CDC investigation team have focused their efforts outside of the hospital: The community contact tracing team retraced Mr. Duncan’s steps after he arrived in the United States and monitored any community members who may have encountered him while he was infectious.
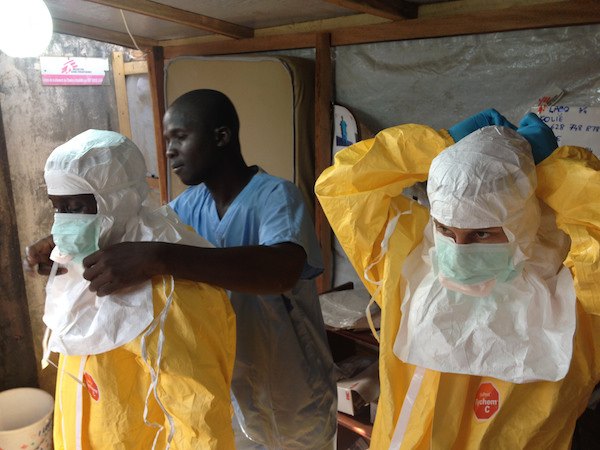
The CDC and the Texas hospital came under scrutiny after two nurses who treated Mr. Duncan at Texas Health Presbyterian contracted Ebola. During congressional hearings, some House members suggested that the CDC did not offer proper personal protective equipment guidelines for health care workers treating the Ebola patient. CDC Director Tom Frieden cited a “breach in protocol” that allowed the nurses to become infected, and he said they may have inadvertently violated protocol by wearing too much protective gear. Both nurses are now hospitalized. Ebola patient Nina Pham is in “good condition” at the National Institutes of Health in Bethesda, Md., and Amber Vinson at Emory University Hospital in Atlanta is “doing OK,” her family says.
Officials also said one of the now-infected nurses called health officials before boarding a plane from Cleveland to Dallas to report having a slightly elevated temperature. However, the CDC cleared her to fly, according to news reports.
The CDC issued new rules for protecting hospitals workers from Ebola on Monday night, saying they must now wear full body coverage suits with no skin showing and must be “repeatedly trained” before treating a patient with Ebola.
Dr. Epstein admits that her experience in Dallas was “stressful,” but she believes that her time on the front line of Ebola has prepared her for a career as a public health leader. She said her experience taught her how to better work with and to trust a large team in the middle of “unexpected challenges.”
Now back in Atlanta, Dr. Epstein is continuing to monitor the Ebola outbreak as well as other long-term surveillance projects related to health care-associated infections.
“I’m really happy to be back,” she said.